Comparison of COVID-19 Dispositions to Circulatory and Respiratory Diagnostic Cohorts
HealthPivots Report
July 6, 2020
In June 2020, CMS released a Preliminary Medicare COVID-19 Data Snapshot[i]. The data are based on services rendered January 1 to May 16, 2020 and are limited to claims received by June 11, 2020. Among the data CMS released in June 2020 were figures on COVID-19 inpatient discharge status. These data are for inpatient claims with a COVID-19 diagnosis listed in any of the 25 diagnosis code fields.
HealthPivots compared these COVID-19 inpatient discharge figures with our own analyses of 2019 Medicare FFS Inpatient claims for acute hospitals. These comparisons examine differences in inpatient mortality, and in post-acute discharge disposition. COVID-19 discharge data are presented alongside all discharges, and the COVID-19 data are compared to data from discharges from two principal diagnosis groups; circulatory and respiratory.
Chart 1, below, presents the inpatient mortality rates in 2019 for Medicare FFS patients with a COVID-19 diagnosis code, all patients from acute hospitals, patients with a circulatory principal diagnosis, and patients with a respiratory principal diagnosis. Table 1 describes the distribution of discharges of these same groups.
Chart 1: Inpatient Mortality (%) Comparison
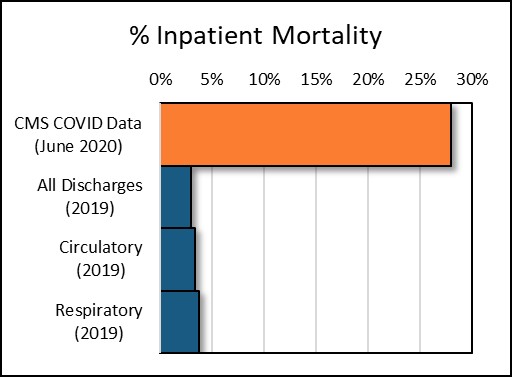
Table 1: Distribution (%) of Inpatient Discharges by Status
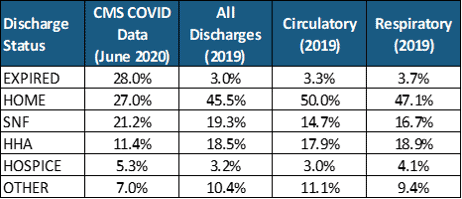
In 2019, inpatient mortality for all Medicare FFS inpatient discharges from acute hospitals was 3.0%. For inpatients with circulatory principal diagnoses and those with respiratory principal diagnoses inpatient mortality was 3.3% and 3.7% respectively. Inpatient mortality in the CMS COVID-19 data was 28.0%. Inpatient mortality for COVID-19 was over 9 times the rate for all inpatients.
Table 2 and Chart 2, below, describe live inpatient discharges and post-acute care discharge disposition. Compared to the circulatory and respiratory diagnosis groups, a higher portion of inpatients with a COVID-19 diagnosis were discharged, live, directly to Skilled Nursing Facilities (SNF) or Hospice, while a lower portion were discharged to home or home health (HHA).
Table 2: Distribution (%) of Live Inpatient Discharges by Status
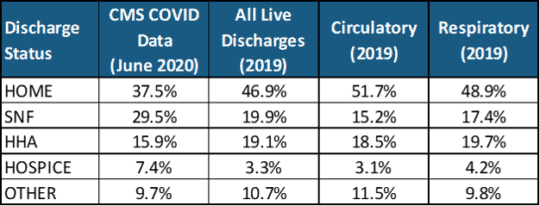
Chart 2: Distribution (%) of Live Inpatient Discharges by Status
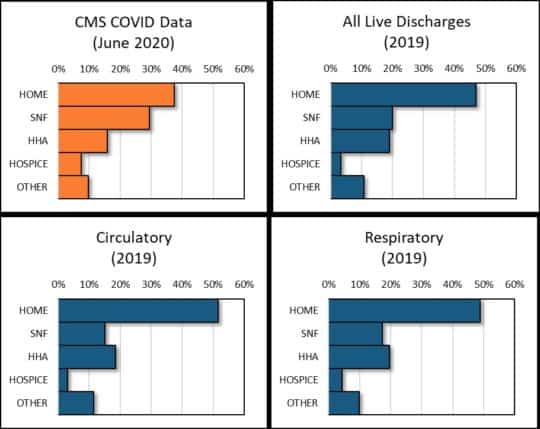
These data indicate COVID-19 inpatients were discharged to advanced care (SNF) and hospice more often compared to an average Medicare FFS live discharge. COVID-19 inpatients were sent to home health (HHA) less often. The following specific differences are observed:
- 29.5% of COVID-19 inpatients were discharged to SNFs, compared with 19.9% of all live discharges, 15.2% of circulatory live discharges, and 17.4% of respiratory live discharges.
- 7.4% of COVID-19 inpatients were discharged to hospice, compared with 3.3% of all live discharges, 3.1% of circulatory live discharges, and 4.2% of respiratory live discharges.
- 37.5% of COVID-19 inpatients were discharged to home, compared with 46.9% of all live discharges, 51.7% of circulatory live discharges, and 48.9% of respiratory live discharges.
- 15.9% of COVID-19 inpatients were discharged to HHAs, compared with 19.1% of all live discharges, 18.5% of circulatory live discharges, and 19.7% of respiratory live discharges.
The findings on SNF and hospice are consistent with the other data released by CMS showing that COVID-19 inpatients were older and had high prevalence of chronic conditions. From these limited data it is not possible to attribute the differences to a specific cause. Pre-existing health conditions, advanced age, the effects of COVID-19, and outbreaks in nursing homes are all likely to contribute to these differences. The specific challenges of care for COVID-19 patients, such as PPE shortages, quarantine requirements, and increased demand for some services may also play an important role. Cases captured by the preliminary CMS data are from concentrated hotspots, whereas the comparison data are national. Regional variation in care patterns may influence the results. Finally, as CMS is clear to point out, as these data are preliminary, they have many limitations.
Data for comparison were extracted from the CMS Chronic Conditions Warehouse in compliance with an executed Data Use Agreement.
[1] Preliminary Medicare COVID-19 Data Snapshot. U.S. Centers for Medicare & Medicaid Services website. Updated June 23, 2020. Accessed July 2, 2020. https://www.cms.gov/research-statistics-data-systems/preliminary-medicare-COVID-19-data-snapshot Citation information: HealthPivots. (2020). Retrieved from https://healthpivots.com, providing sophisticated analytics examining performance geographically or by provider in all aspects of the post-acute health system
